What is diabetes?
When a food containing carbohydrate is eaten, your body digests the carbohydrate into sugar (called glucose), which can then be used as energy by the cells in your body. Diabetes is a condition that arises when your body can’t properly control the amount of glucose in your blood.
A hormone called insulin is needed to transfer glucose from the bloodstream to cells and be converted to energy. For people with diabetes, blood glucose levels are often higher than normal because either the body does not produce insulin (type 1 diabetes) or cannot manage insulin properly (type 2 diabetes).
High levels of glucose in the bloodstream can lead to short term complications such as:
- passing large amounts of urine
- being extremely thirsty and drinking lots of fluids
- being tired
- having blurred vision
- having frequent skin infections, which are slow to heal
Controlling diabetes is important to prevent serious long-term complications such as:
- heart and circulation problems
- infections
- kidney disease
- eye problems, which can lead to blindness.
- nerve damage to the lower limbs and other parts of the body
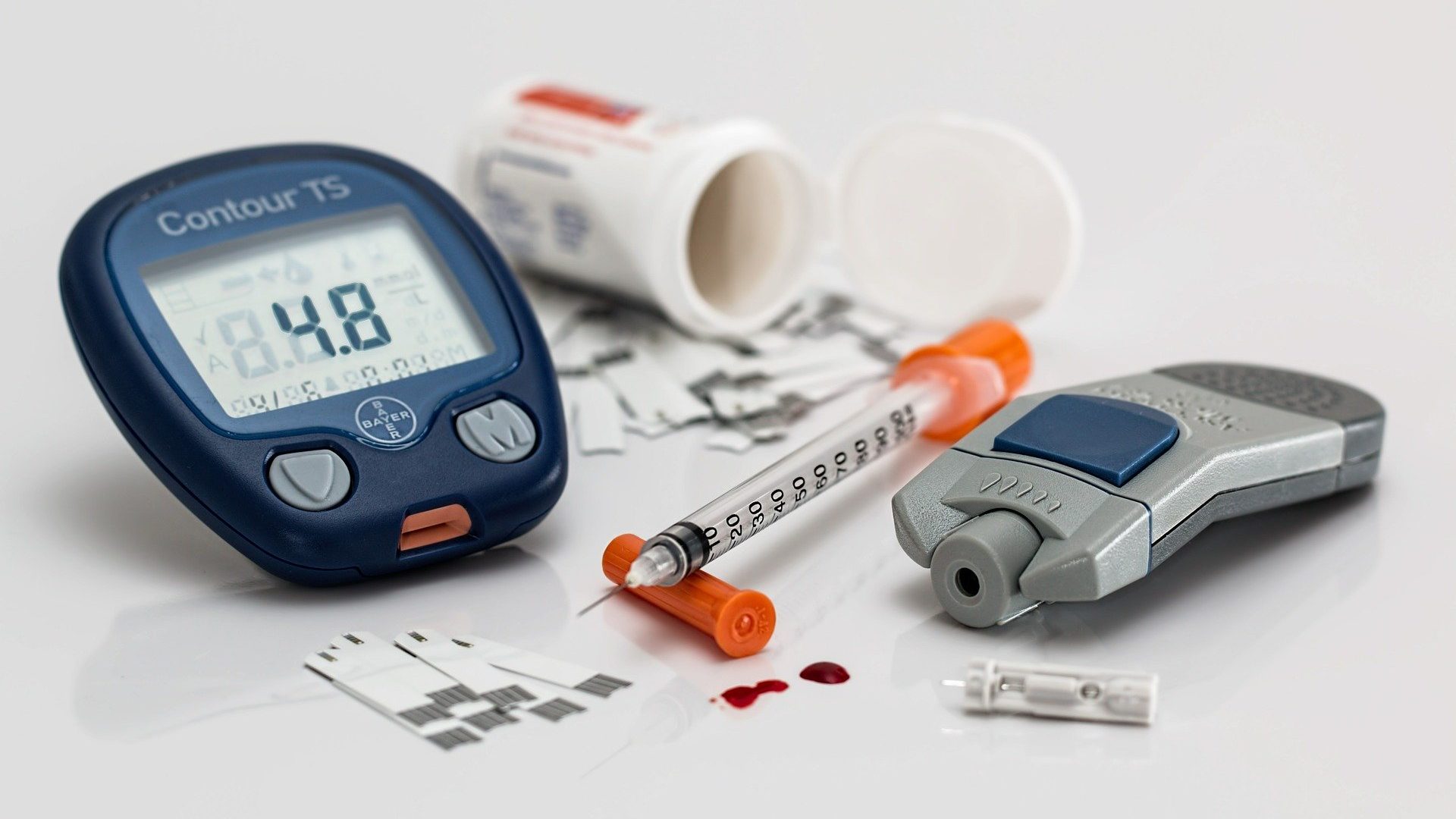
Remember:
- Diabetes develops when your body is unable to maintain healthy levels of glucose in the blood.
- High levels of glucose in the bloodstream can lead to short term complications.
- Controlling diabetes is important to prevent serious long-term complications.
Types of diabetes
There are three main types of diabetes:
Type 1 diabetes
Type 1 diabetes is an autoimmune condition caused by the pancreas failing to produce insulin and accounts for 10-15% of all diabetes cases in Australia.1 It can appear at any age, but most commonly presents in childhood and early adult life. People with type 1 diabetes cannot produce enough insulin, and therefore they must inject themselves with insulin several times a day.
There is currently nothing that can be done to prevent or cure type 1 diabetes.
Type 2 diabetes
Type 2 diabetes is the most prevalent form of diabetes and accounts for 85-90% of all diabetes cases in Australia.1 Type 2 diabetes occurs when the cells in the body develop insulin resistance. Diagnosis is usually in older adults, but it is becoming more common in adolescence and even children. The causes are unknown, but the risk is increased by having a family history, aging, having prior gestational diabetes, having pre-diabetes, being above the healthy weight range and an inactive lifestyle.
There is no cure for type 2 diabetes, but if you are at risk, you can delay and sometimes prevent developing type 2 diabetes by embracing a healthy lifestyle. This includes regular exercise, eating a balanced diet and maintaining a healthy weight.
Gestational diabetes
Gestational diabetes occurs during pregnancy. Approximately 12-14% of pregnant women will develop it around the 24th-28th week mark.1 The hormonal changes of pregnancy combined with a predisposition for poor insulin production or utilisation, results in increased blood glucose levels in the mother and the baby. For most women with gestational diabetes, the diabetes will disappear after the baby is born. However, 30-50% of women who have gestational diabetes go on to develop type 2 diabetes later in life.
Remember:
- Type 1 diabetes is an autoimmune condition and accounts for 10-15% of all diabetes cases in Australia.
- Type 2 diabetes is the most prevalent form of diabetes and accounts for 85-90% of all diabetes cases in Australia.
- Gestational diabetes occurs during pregnancy. Approximately 12-14% of pregnant women will develop it around the 24th-28th week mark.
Managing diabetes
For all diabetics, regular physical activity and a healthy, balanced diet is key to well-controlled blood glucose levels. Insulin users also need to consider the timing, amount and type of carbohydrate foods they eat, as well as the timing, amount and type of insulin they take. Regular blood glucose testing will help manage your diabetes, but all diabetics should consult regularly with their diabetes health team. All people with diabetes should avoid smoking.
Healthy eating tips for people with diabetes
A healthy diet used in the treatment of diabetes is similar to the diet recommended for all Australians. To help manage your diabetes, Diabetes Australia recommend that you:
- Eat regular meals and healthy snacks spread over the day.
- Base meals on high fibre, low GI carbohydrate foods such as wholegrain breads and cereals, beans, lentils, vegetables and fruits.
- Watch the amount of fat you eat and limit the amount of saturated fat by choosing lean meats and healthy fats. Try to avoid fried takeaway foods, pastries and biscuits.
- Keep your weight within the healthy weight range by matching the amount of food you eat with the amount you burn up each day (see energy in/energy out fact sheet).

Beef, barley and vegetable soup
Looking for a meal with high fibre wholegrains and packed full of vegetables? Try this hearty beef, barley and vegetable soup.
Remember:
- Regular physical activity and a healthy, balanced diet is key to well-controlled blood glucose levels.
- All diabetics should consult regularly with their diabetes health team.
- All people with diabetes should avoid smoking.
Carbohydrates and the glycaemic index
The amount of carbohydrate in a meal is the most important factor influencing blood glucose levels after a meal. Foods containing carbohydrate include breads, cereals, rice, pasta, grains such as barley and couscous, fruit and fruit juices, legumes and some vegetables such as potato, sweet potato and corn. Milk and yogurt are also a source of carbohydrate in the form of the milk sugar, lactose.
The glycaemic index (GI) is a useful tool to choose foods to help control blood glucose levels in people with diabetes. Carbohydrates in food are digested and absorbed at different rates. The GI is a way of ranking carbohydrate-containing foods (from 0-100) based on whether they raise blood sugar levels a lot, moderately, or a little. Carbohydrate containing foods that are digested quickly will result in a high blood glucose level and have a high glycaemic index (high GI foods). Foods with a GI 70 and above are classified as high GI foods.
Carbohydrate foods that are digested more slowly raise blood glucose levels more slowly, so have a lower glycaemic index (low GI foods). Foods with a GI 55 and below are low GI foods. Eating foods with a low GI can help people with diabetes control their blood glucose levels. Eating moderate amounts of low GI carbohydrate foods regularly over the day will help you maintain consistent blood glucose levels. Low GI foods also stop you from feeling as hungry, which may help you to manage or lose weight.
Healthy, low GI food choices
- Milk and dairy foods – reduced or low-fat varieties of milk and dairy foods are the best choices for people with diabetes.
- Bread – wholegrain, fruit loaf and sourdough.
- Breakfast cereals – traditional porridge, natural muesli and some high fibre varieties.
- Pasta and noodles – all varieties.
- Some varieties of rice – ‘Basmati’ and ‘Doongara’ varieties are moderate to low GI.
- Grains – barley, bulgur and semolina.
- Legumes – beans (e.g. baked beans, kidney beans, soy beans), peas and lentils.
- Fruit – apple, orange, pear, peach, grapes, kiwi fruit, banana, plums.
- Vegetables – most vegetables have low amounts of carbohydrate and therefore have little effect on your blood glucose levels.
*Vegetables with a significant amount of carbohydrate include potato, sweet potato, yams and sweet corn. Orange sweet potato, yams and sweet corn are the lower GI choices.
Remember:
- The amount of carbohydrate in a meal is the most important factor influencing blood glucose levels.
- The glycaemic index (GI) is a useful tool to choose foods to help control blood glucose levels.
- Eating moderate amounts of low GI carbohydrate foods regularly over the day will help maintain consistent blood glucose levels.
The role of dairy foods in diabetes

As one of the core food groups, dairy foods play a key role in a healthy balanced diet. Dairy foods (such as milk, cheese and yogurt) provide essential nutrients, including:
- Protein
- Carbohydrate
- Vitamins (A, D, B12 and riboflavin)
- Minerals (calcium, phosphorus, magnesium, potassium and zinc)
Because they have a low GI, dairy foods are an ideal food for people with diabetes. In addition, research suggests that including dairy foods as part of a healthy lifestyle might help reduce the risk of developing diabetes.
There is a wide range of reduced or low-fat dairy foods which are ideal for calorie-controlled diets or people who need to limit their saturated fat intake. Including the recommended serves of dairy every day into your diabetes management plan is easy with dairy’s great taste and versatility. One serve is equal to:
- One glass (250mL) of milk
- A tub (200g) of yogurt
- 2 slices (40g) of cheese
Nutrition Australia would like to acknowledge Dairy Australia as the original author of this resource.
- https://www.ndss.com.au/about-diabetes/resources/find-a-resource/understanding-type-1-diabetes-fact-sheet/ (Accessed July 2020)
Produced by Nutrition Australia Vic Division, October 2014. Reviewed August 2021.




